Mechanical Thrombectomy for Stroke
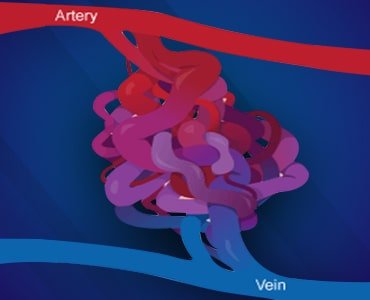
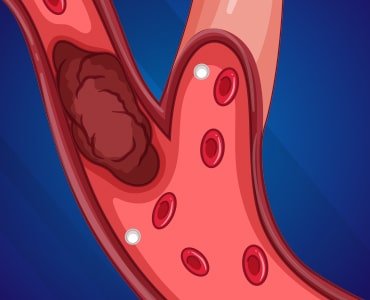
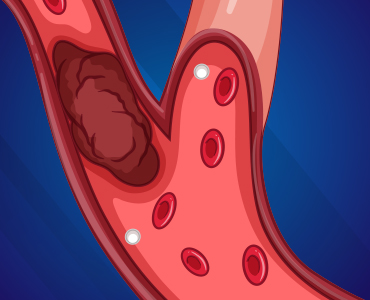
A stroke is a condition where the blood supply to the part of the brain is reduced or blocked, depriving brain cells of nutrients and oxygen. Because of this, the brain cells begin to die within a few minutes. Thus, stroke is a medical emergency that needs prompt treatment to prevent brain damage and other complications.Blood clots in a blood vessel supplying the brain are one of the most common causes of stroke. Fortunately, a minimally invasive procedure is available to remove these clots from the vessels: mechanical thrombectomy.Let’s understand more about this procedure and how it helps people with stroke.
Mechanical Thrombectomy
It is a type of minimally invasive procedure in which an interventional neuroradiologist removes the clot using special equipment. The doctor makes a very tiny hole or an incision in the groin or the wrist to access the blocked vessel.

The doctor threads a catheter through the artery to reach the clot under the guidance of fluoroscopy (continuous x-ray). Next, they can introduce a stent retriever (a stent-like device) to reach the clot through the catheter.
The stent retriever pushes through the blood clot, expanding the blood vessel. As the stent retriever captures the blood clot, the doctor will pull it out, removing the clot.
So, mechanical thrombectomy aids in stopping the damage entirely or to some extent by removing the clot that was clogging the artery supplying the brain.
Before doing the Mechanical Thrombectomy the doctor will use imaging techniques such as MRI and CT scans to help understand if mechanical thrombectomy can help.
Usually, this procedure needs to be carried out within 6 to 24 hours. In cases where the patient reaches the hospital within four and a half hours, a drug called tissue plasminogen activator (a drug to break down the clot) may be used in addition to this technique.
Benefits
The effect of the procedure is almost immediate. In some cases, the patient even becomes mobile again or starts speaking immediately. However, other patients may take weeks to months to improve.
Risks
Like any other procedure, mechanical thrombectomy may also have some risks. However, If done by a trained professional these risks are minimal. Some common ones include:
- Damage to the blood vessels
- Bleeding
- Infection
- Reactions or problems to anesthesia
- Clot traveling deeper into the vessel
Despite the risks, mechanical thrombectomy lowers the risk of stroke complications and improves the chances of survival. American Heart and Stoke association has recommended this treatment for the stroke patients. The procedure is thus widely used to manage stroke.