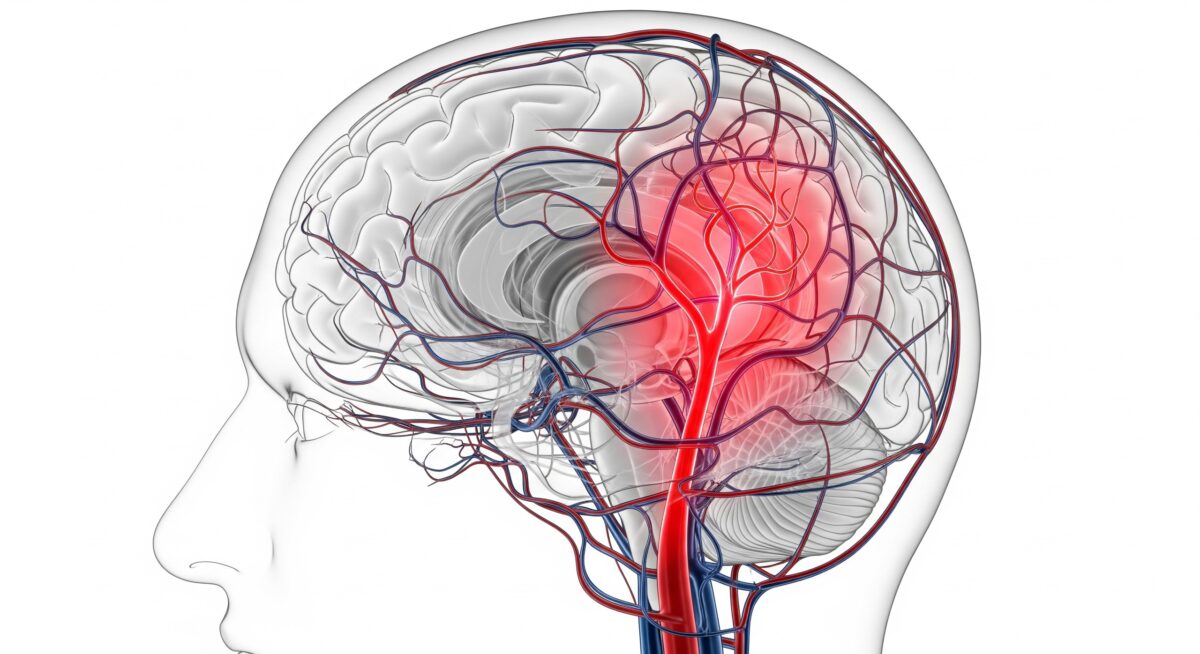
A sudden severe headache can be alarming, especially when it feels unlike anything you’ve experienced before. While many headaches are harmless, some can indicate a serious medical emergency. As explained by Dr. Vivek Gupta, recognizing the difference is crucial, as a brain hemorrhage—also known as brain bleeding—requires immediate attention.
Often described as a “thunderclap headache,” this type of pain reaches its peak intensity within seconds or minutes. Unlike regular headaches, it may be accompanied by other brain hemorrhage symptoms such as nausea, vomiting, confusion, blurred vision, or even loss of consciousness. Understanding these warning signs of brain hemorrhage can help you act quickly and potentially save a life.
What Causes a Sudden Severe Headache?
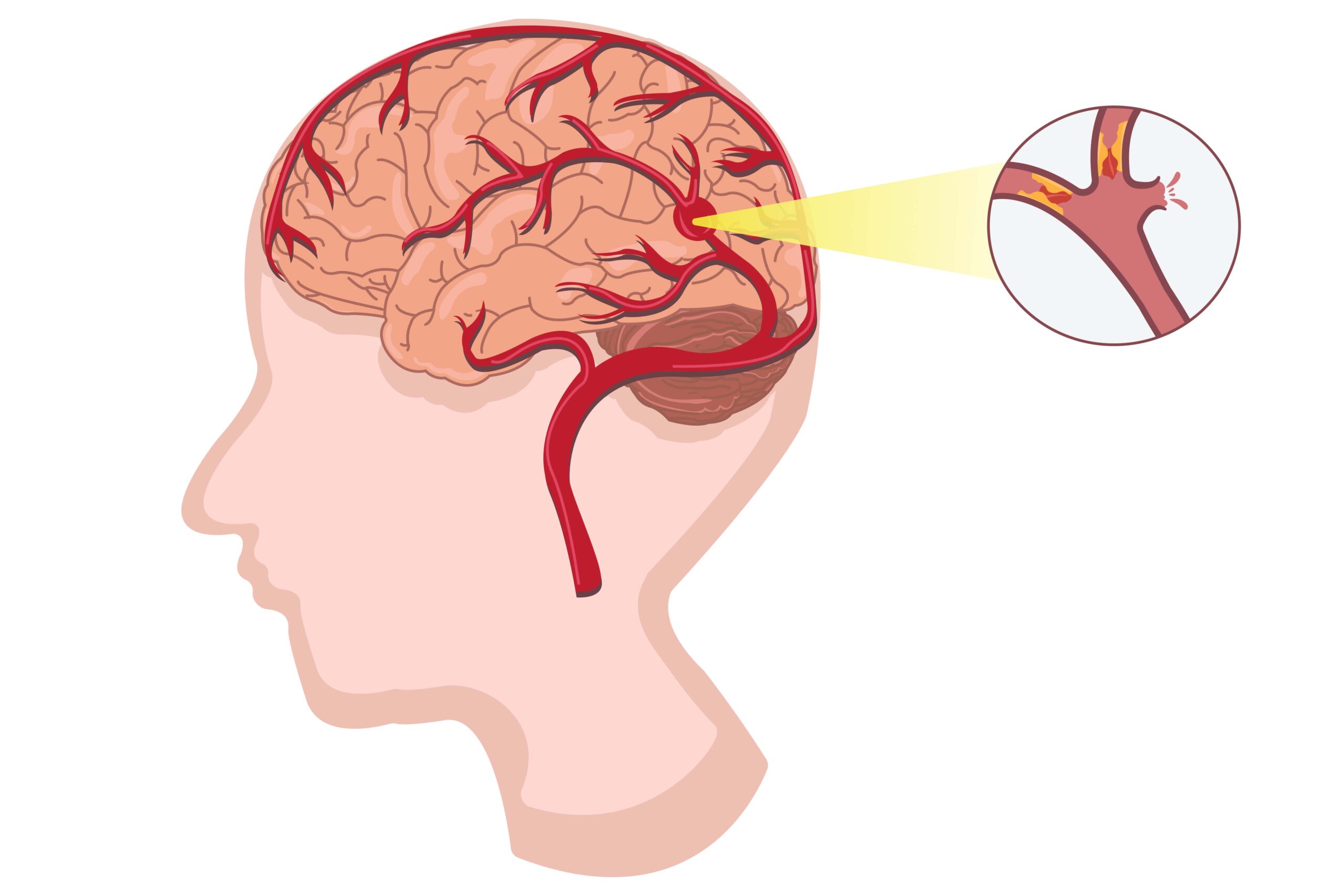
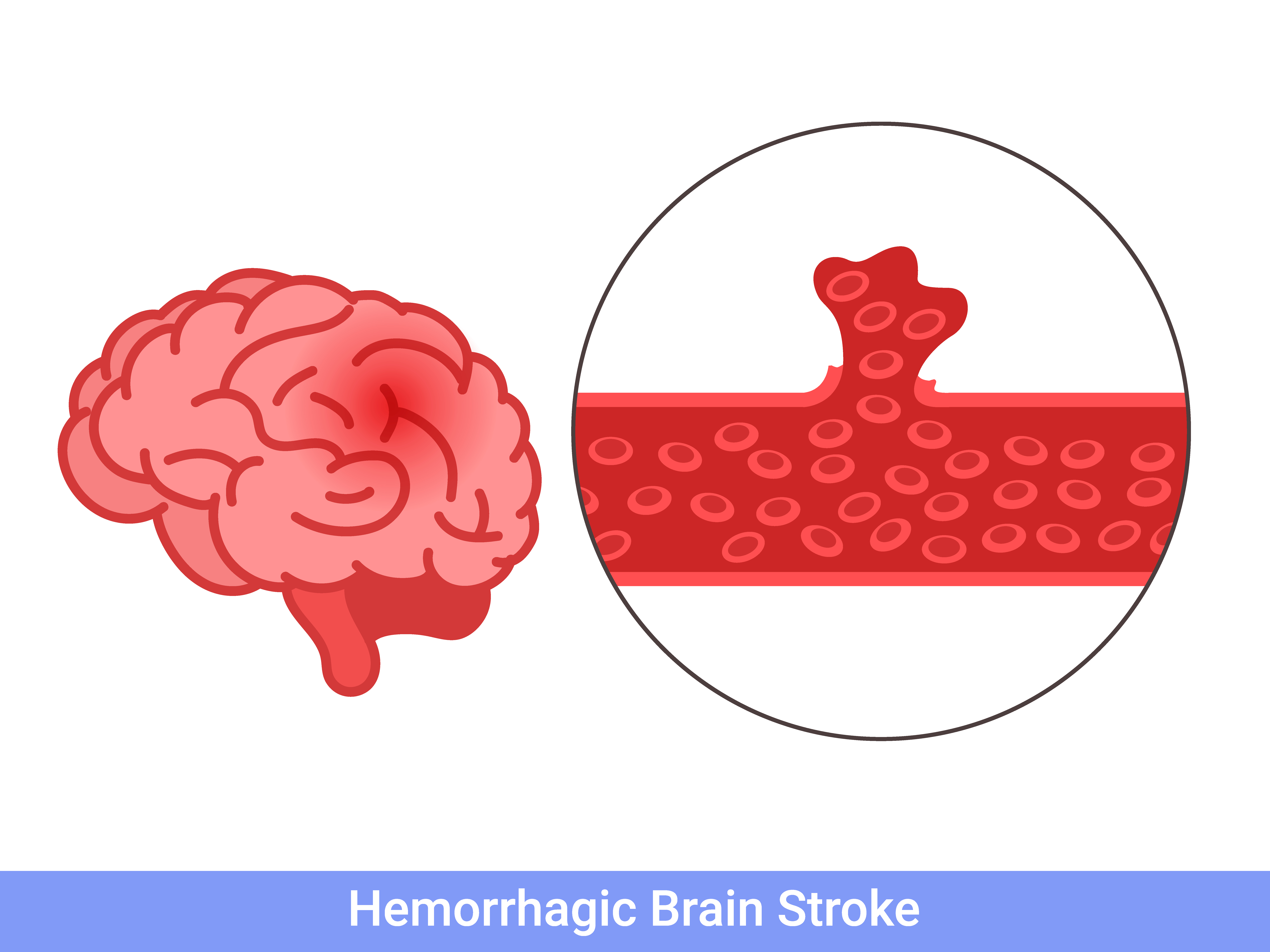
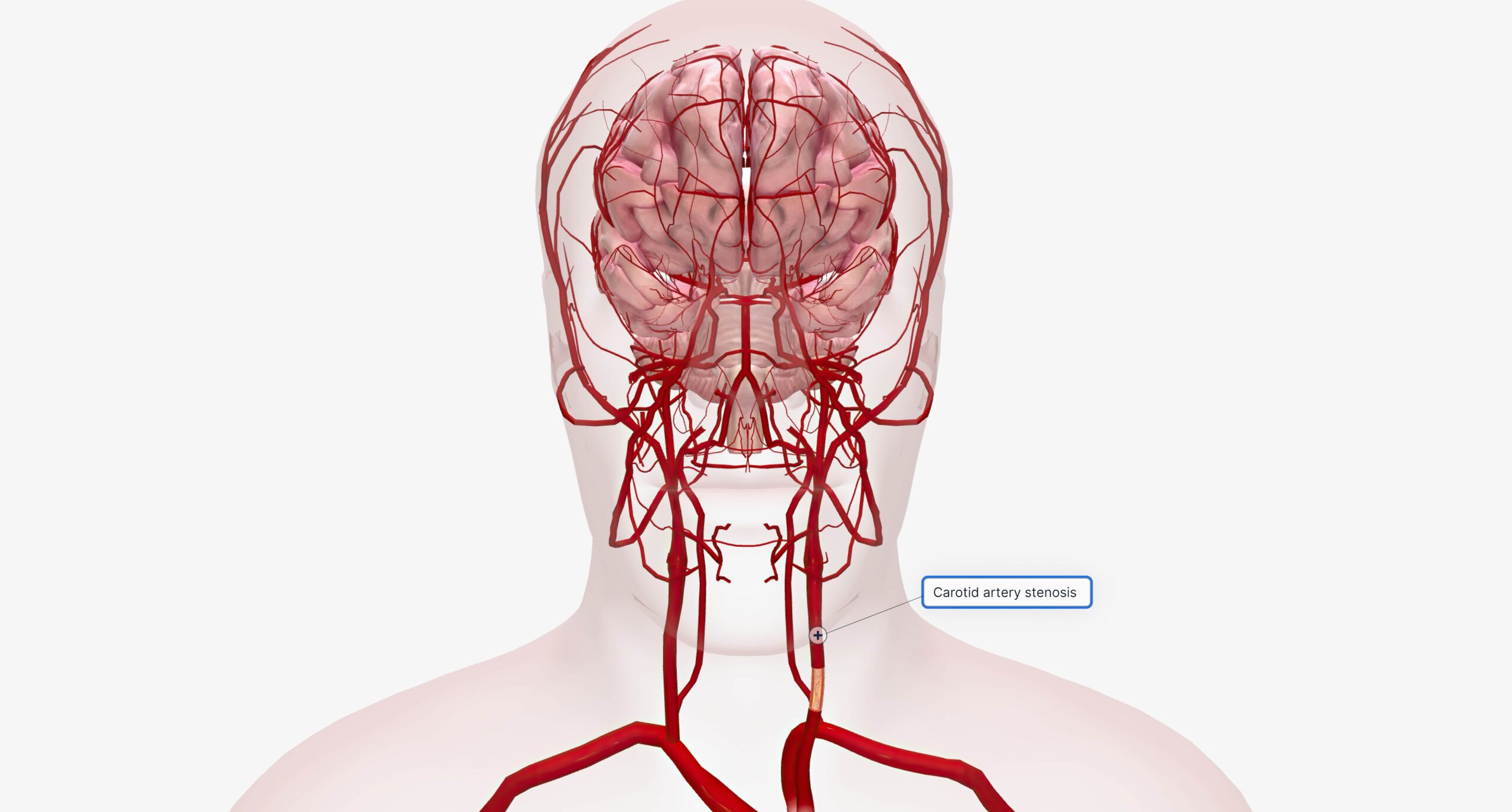
There are several severe headache causes, but when it comes to brain bleeding, common triggers include high blood pressure, head injury, aneurysm rupture, or blood vessel abnormalities. People with uncontrolled hypertension are at a higher risk, making it essential to monitor and manage blood pressure levels regularly.
In some cases, a sudden headache may also be linked to conditions like migraines or tension headaches. However, the key difference lies in the intensity and sudden onset. If a headache feels unusually severe or different from your typical pattern, it should never be ignored.
When Is a Headache an Emergency?
Knowing when a headache is serious can make all the difference. Seek immediate medical help if the headache is:
- Sudden and extremely intense
- Accompanied by neck stiffness or fever
- Paired with confusion or difficulty speaking
- Associated with weakness, numbness, or seizures
- Occurring after a head injury
These headache emergency signs may indicate a brain hemorrhage or another life-threatening condition. Prompt diagnosis and treatment are critical to prevent complications.
Risk Factors You Should Not Ignore
Certain individuals are more vulnerable to brain bleeding. Common risk factors for brain hemorrhage include:
- High blood pressure
- Smoking and excessive alcohol use
- Blood-thinning medications
- Family history of vascular conditions
- Advanced age
By addressing these factors, you can reduce your risk and protect your overall brain health.
Act Fast, Stay Safe
A sudden severe headache is not something to take lightly. Being aware of brain bleeding symptoms and acting quickly can significantly improve outcomes. Early intervention not only saves lives but also reduces the chances of long-term complications.
At the forefront of advanced neurological care, Dr. Vivek Gupta offers expert evaluation and timely treatment for conditions like brain hemorrhage. Don’t ignore the signs—book your consultation for expert care.